The Gut Keeps Time
What a Startup Founder Taught Me About Sleep, Microbes, and the Molecular Clock
At 10:30 p.m., Abby’s house is finally quiet.
This is when her second shift begins.
The dishwasher hums in the kitchen. Outside, the cul-de-sac is dark, the streetlight casting a pale circle onto empty pavement. Abby closes her children’s bedroom door and stands for a moment in the hallway, listening. Five and seven now. The last time they were in Hawaii they were three and five, barefoot and salt-streaked, their hair nearly white in the sun.
Her office doubles as the guest room. A fitted sheet hangs half-folded over the bed. A small pile of laundry waits near the pillows. The desk is wedged into the corner beneath the window, just wide enough for her laptop and a second monitor.
She rests her palm on the lid before opening it.
The screen saver flickers to life. Hawaii. Late afternoon light. Younger children. Then the login prompt replaces it. Slack notifications bloom in the corner of the screen.
Her body feels ready for sleep. Her shoulders ache. There is a knot in her left trapezius that has lived there for weeks. But her mind will not release tomorrow’s fundraising presentation. Slides reorder themselves behind her eyes.
She has already had two coffees today. One at 6:15 a.m. in a travel mug while packing lunches. Another at three in the afternoon when her focus began to thin. The second one sat heavier.
When she leans forward, she feels the familiar pressure beneath her ribs. Not sharp pain, but fullness. Inflation. For weeks her abdomen has felt swollen, unsettled. Mornings bring the vague dissatisfaction of an incomplete bowel movement. Something stalled. Something off.
I meet her in my clinic waiting room.
The television is off. Travel magazines fan across the coffee table. She flips through one slowly, not reading, just turning pages.
“Ready to come back?” I ask.
She tilts her head and smiles. “Not really. I like this quiet time.”
In the exam room, she drops into the cushioned chair angled toward the window. The fluorescent lights hum overhead.
“Could we use natural light?” she asks.
I switch them off. The room exhales.
Her watch vibrates. She taps it silent without looking.
“How’s your sleep?” I ask.
She smirks. “Ask me that in eighteen years, when my kids are out of the house.”
I smile but press gently. “What time did you go to bed last night?”
She makes the grimace emoji in real life. “Twelve-thirty. I had to finish the slide deck.”
“And what time were you up?”
“Six. The little stinkers were climbing into my bed.”
She shifts in the chair.
“I just feel gross,” she says. “Inflamed. Bloated. My bowels are all over the map.”
I ask about timing. She says her gut has always been sensitive, but two weeks ago the startup’s funding began to thin. She was asked to assemble a high-stakes pitch deck. That is when it intensified.
As she talks, I think about seams.
The intestine is a wall only one cell thick. The epithelial cells stand shoulder to shoulder, stitched together by tight junction proteins such as occludin and claudin. These molecular fasteners regulate what passes from the gut into the bloodstream. Nutrients are allowed through. Microbes are confined.
-The immune system does not tolerate ambiguity.
When the seams between cells loosen, it responds as if something is wrong, even if nothing visible has entered.
“But I’ve been eating really clean,” she says. “No processed food. No sugar. I even cut gluten. How could this be happening?”
“What does clean look like?” I ask.
“Smoothies. Spinach. Protein powder. Salad for lunch. Grilled chicken. Vegetables. I’m not eating garbage.”
“That all sounds intentional,” I say. “But food is only one component of gut health.”
She studies my face. “I know what you’re going to tell me. And I don’t want to hear it.”
“I’m not here to shame your schedule,” I tell her. “I just want to explain what your body is doing.”
She leans back, guarded but listening.
“There is a molecular timekeeper in your gut that helps regulate inflammation and reinforce the barrier at night. It is most active when you sleep. It is called NR1D1.”
I pause. “It reminds me of R2D2.”
She laughs softly.
“Think of it as the night supervisor. When sleep is repeatedly shortened, that supervisor clocks out early. The seams are not reinforced the way they should be.”
I explain that sleep loss also shifts the balance of bacteria living in the gut. Certain microbes that produce anti-inflammatory compounds decrease. Others expand.
“One compound in particular tends to drop with chronic sleep disruption,” I say. “Taurine. It is microbiota-derived. It helps stabilize the barrier and supports that timekeeper.”
She looks down at her hands and sinks deeper into the chair.
“So I’m not imagining it.”
I shake my head.
“Guess I’m the poster child for NR1D1,” she says, attempting a smile.
After she leaves, I return to the literature. (Wang,et.al 2025)
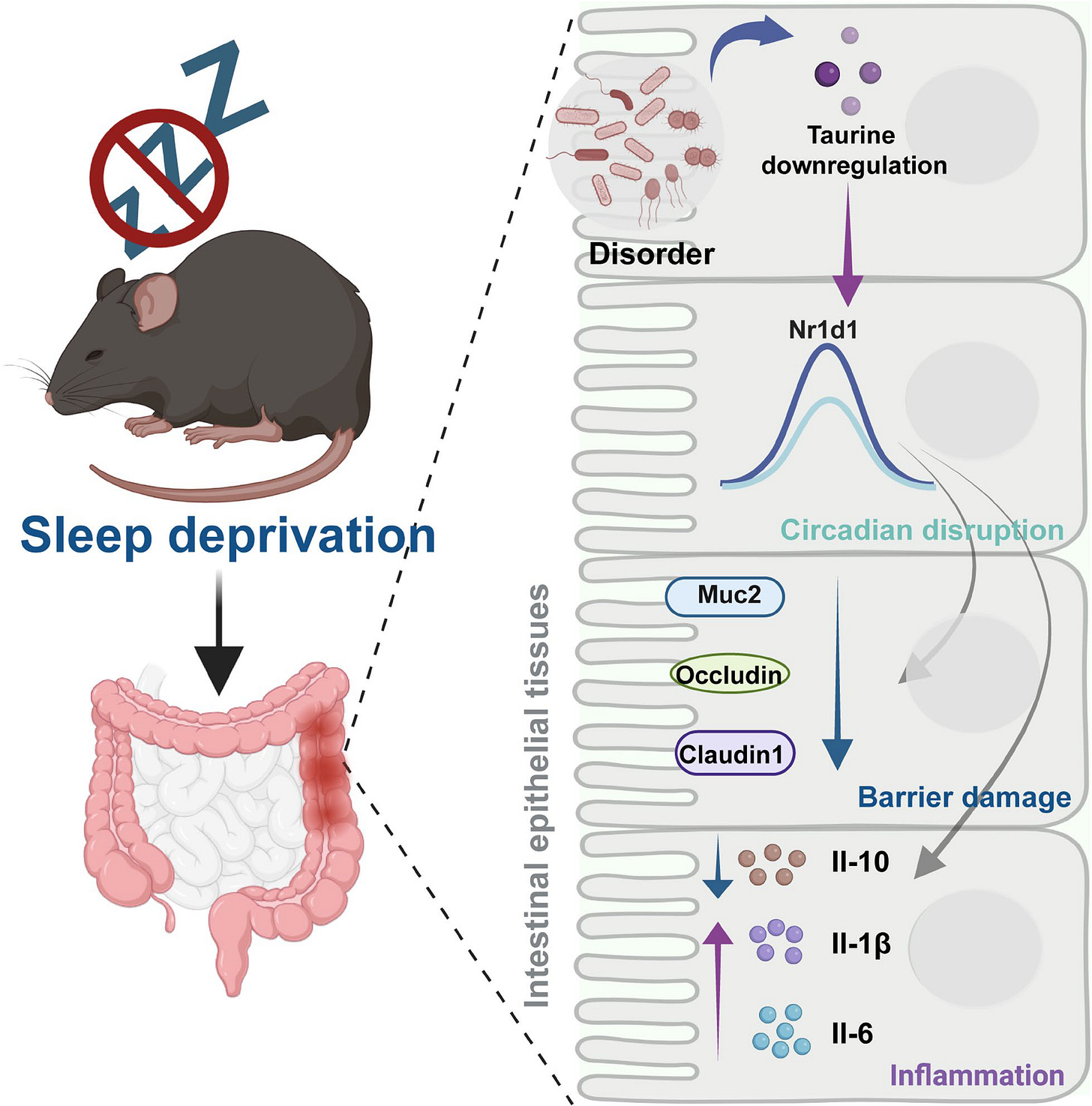
In one experiment, mice are allowed only four hours of sleep a night for three weeks. The apparatus is mechanical. Rotating rods turn just fast enough to prevent sustained sleep.
By the end of the protocol, their colons are shorter. Inflammatory infiltration increases. Tight junction proteins such as occludin and claudin-1 are reduced. The seams are weaker.
Transcriptomic analysis reveals suppression of NR1D1, a core regulator of the intestinal circadian rhythm. When NR1D1 falls, the downstream balance shifts. The barrier loses reinforcement during the very hours it is meant to repair.
Untargeted metabolomics identifies a drop in taurine. When taurine is restored, NR1D1 expression rebounds. Tight junction proteins increase. Inflammation quiets.
Sleep deprivation stacked for days is not abstract. It is mechanical. It is measurable.
source:Wang, Z., Zhou, L., Zheng, Y., Zhong, X., Huang, R., Sun, W., … & Li, W. (2025). Nuclear receptor Nr1d1 links sleep deprivation to intestinal homeostasis via microbiota-derived taurine. Journal of Translational Medicine, 23(1). https://doi.org/10.1186/s12967-025-07089-8
The intestine keeps time.
When I was in medical school, my professor Dr. Keefer warned us about something he called bring-it-itis. It was the belief that effort could outmaneuver physiology. That optimization could replace rest.
“You can’t trick the gut,” he would say. “Not if it’s overstressed and under-rested.”
Abby is not reckless. She is disciplined. But discipline without rest becomes its own stressor.
She leans forward in the chair.
“What if I treat this like a sprint?” she says. “Two weeks. Laptop closed by ten-thirty. No exceptions. I’ll see if my performance tanks.”
It sounds like something a founder would say. Not surrender. Experiment.
She asks if there is anything she can take that will not sedate her or fog her brain.
I tell her there is emerging evidence that taurine, sometimes paired with glycine, may support barrier integrity and circadian signaling. But it is not a substitute for sleep. It works best when the rhythm is restored.
That night, at 10:28 p.m., Abby stands again in the guest-room office. The unfolded laundry is still on the bed. The cul-de-sac is quiet.
The Hawaii screen saver glows briefly before the login prompt appears. Her hand rests on the lid.
She closes the laptop.
Somewhere in the dark, a molecular supervisor waits for its shift.
Biology does not negotiate. It waits.
If this resonated with you, ask yourself one question tonight:
What time does your gut think it is?
Source: Wang, Z., Zhou, L., Zheng, Y., Zhong, X., Huang, R., Sun, W., … & Li, W. (2025). Nuclear receptor Nr1d1 links sleep deprivation to intestinal homeostasis via microbiota-derived taurine. Journal of Translational Medicine, 23(1). https://doi.org/10.1186/s12967-025-07089-8
Related post